EMS Naloxone Leave-Behind
Jump to:
Resources for EMS Clinicians,
Studies and Best Practices
What is EMS Naloxone
Leave-Behind?
Naloxone leave-behind is a collaboration between public health and public safety that allows EMS clinicians to leave naloxone on-scene with patients and their support system.
Research shows overdose survivors face a significantly increased risk of fatally overdosing in the future. EMS personnel can help reduce the risk of fatal overdose by giving naloxone kits directly to at-risk patients and their family, friends, and roommates.
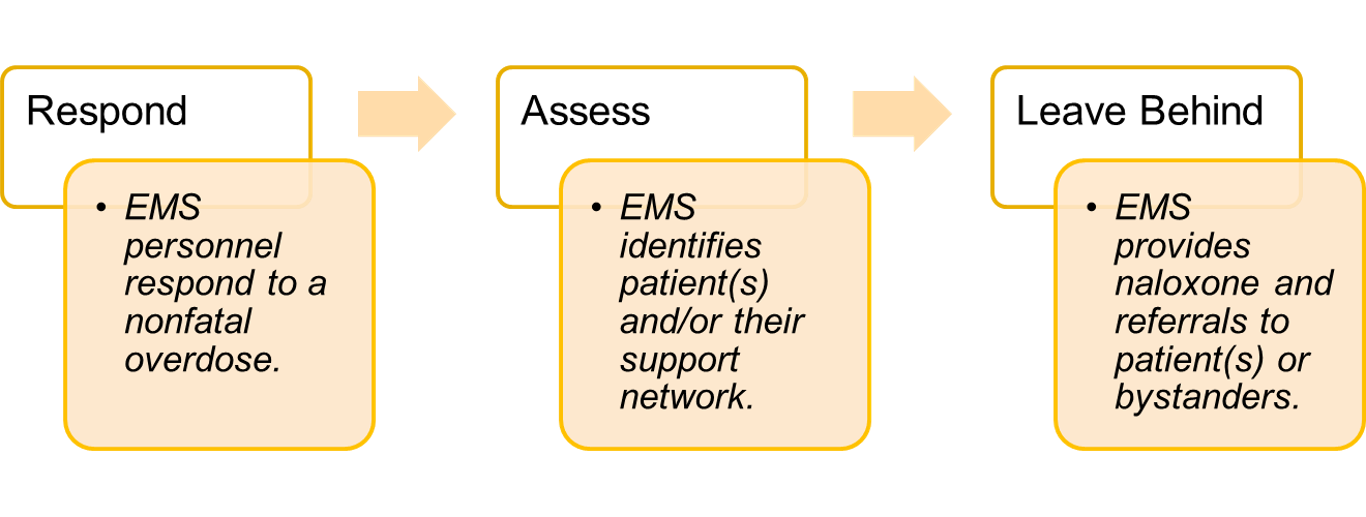
Why do Naloxone Leave-Behind?
Naloxone leave-behind programs improve linkages to care in the community, which can reduce future overdoses and the strain on the EMS workforce.
Naloxone is provided at no cost to EMS agencies by the state of Maryland. While naloxone is not the sole answer to the overdose crisis, it can help patients live another day, improve community health, and prevent overburdening healthcare systems.
Naloxone leave-behind allows EMS professionals to give naloxone to the people who need it the most. By providing these kits, EMS can save lives beyond the patient care given in the moment after an overdose.
Benefits of Leave-Behind
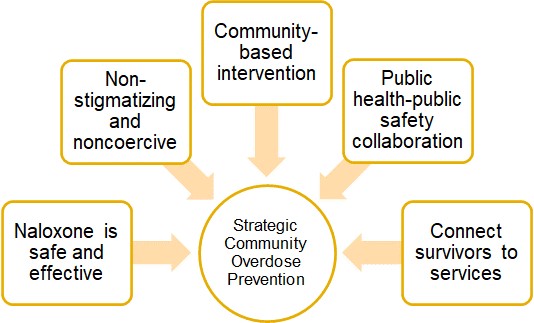
Leave-behind allows clinicians to provide life-saving resources whether a patient accepts transport or not. In the long term, connecting patients to resources can make your job as an EMS clinician easier.
First responders are uniquely positioned to interrupt the cycle of nonfatal-to-fatal opioid overdose by increasing distribution of overdose prevention resources to patients in real time.
Leave-behind kits can also connect patients to
300+ organizations that can dispense naloxone refills in every Maryland county.
Leave-Behind in Maryland
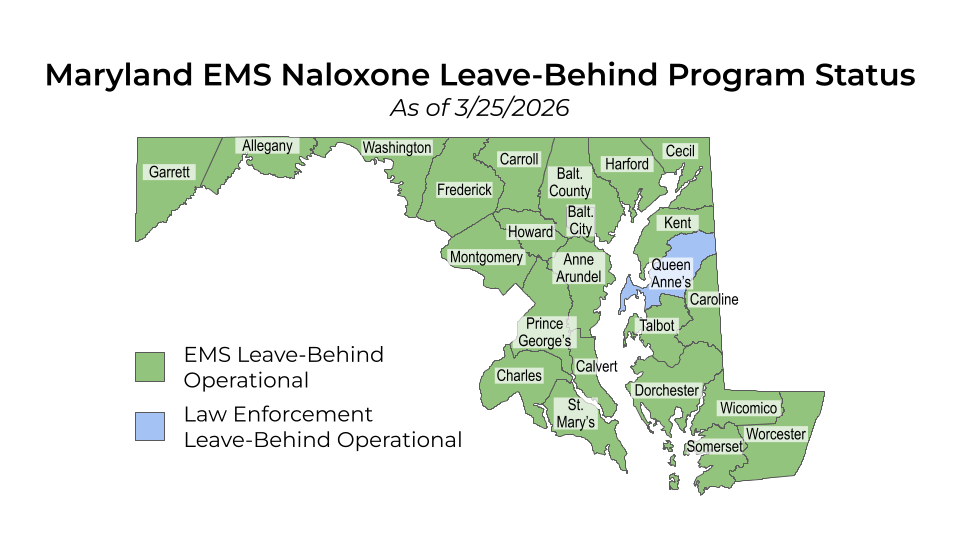
Maryland’s leave-behind program is here to stay. Since July 2025, Maryland's EMS medical protocols have allowed all Maryland EMS agencies to participate by default. Between 2018 and June 2025, the program was opt-in by county.
Since 2018, EMS leave-behind programs have distributed over 62,000 doses of naloxone to over 27,000 Marylanders. For the most up-to-date Maryland EMS naloxone leave-behind data, visit the MDH Overdose Dashboard.
Leave-behind programs have proven successful across multiple states.
Resources for EMS Clinicians
Video: Jason Patton on Post-Overdose Outreach
This 3-minute video explains the unique ability first responders have to intervene post-overdose, and why hope is never out of reach.

